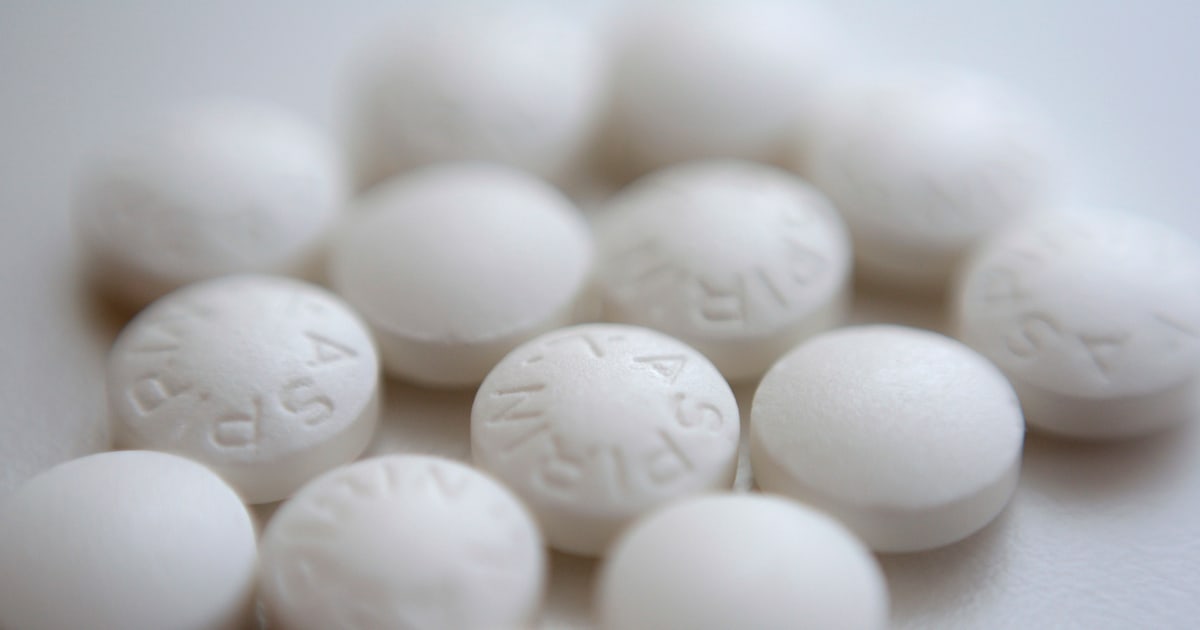
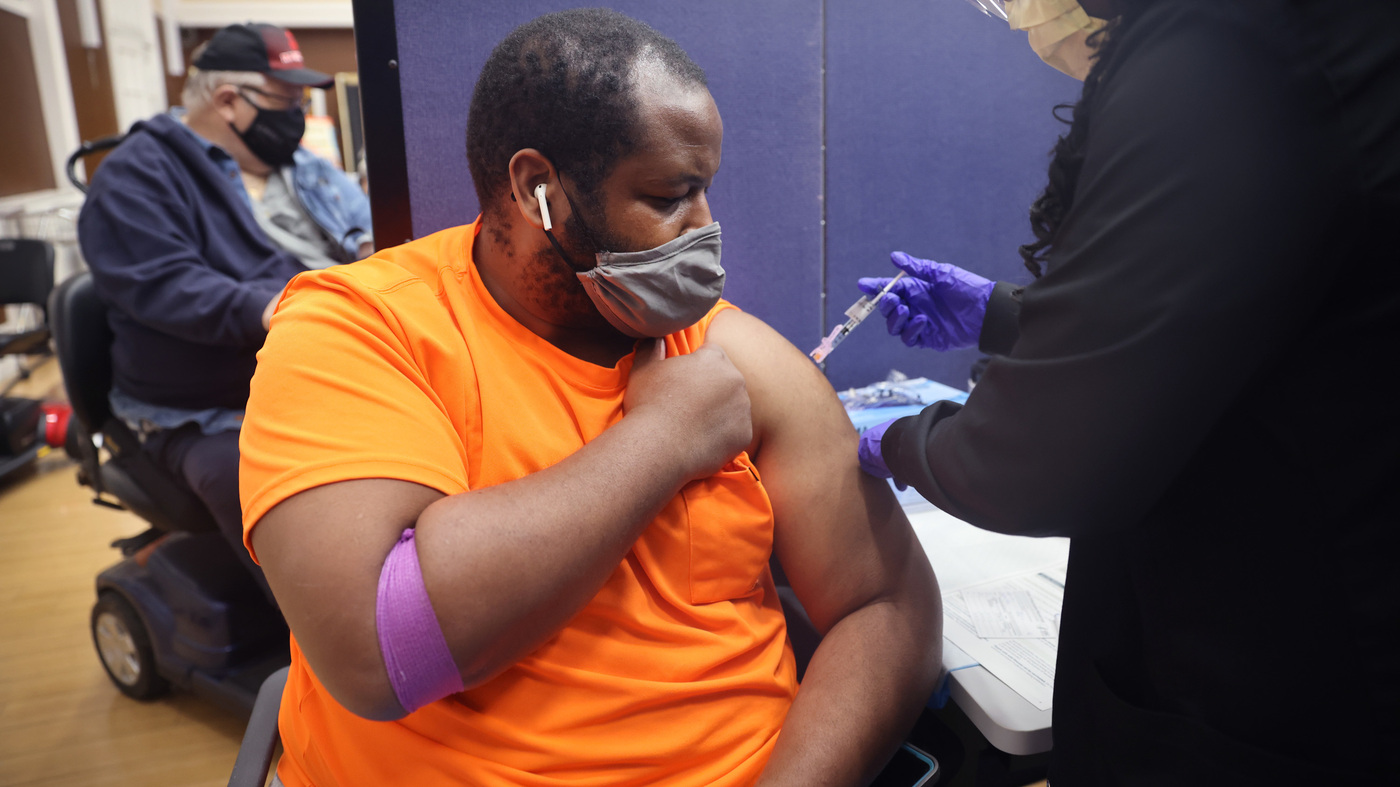
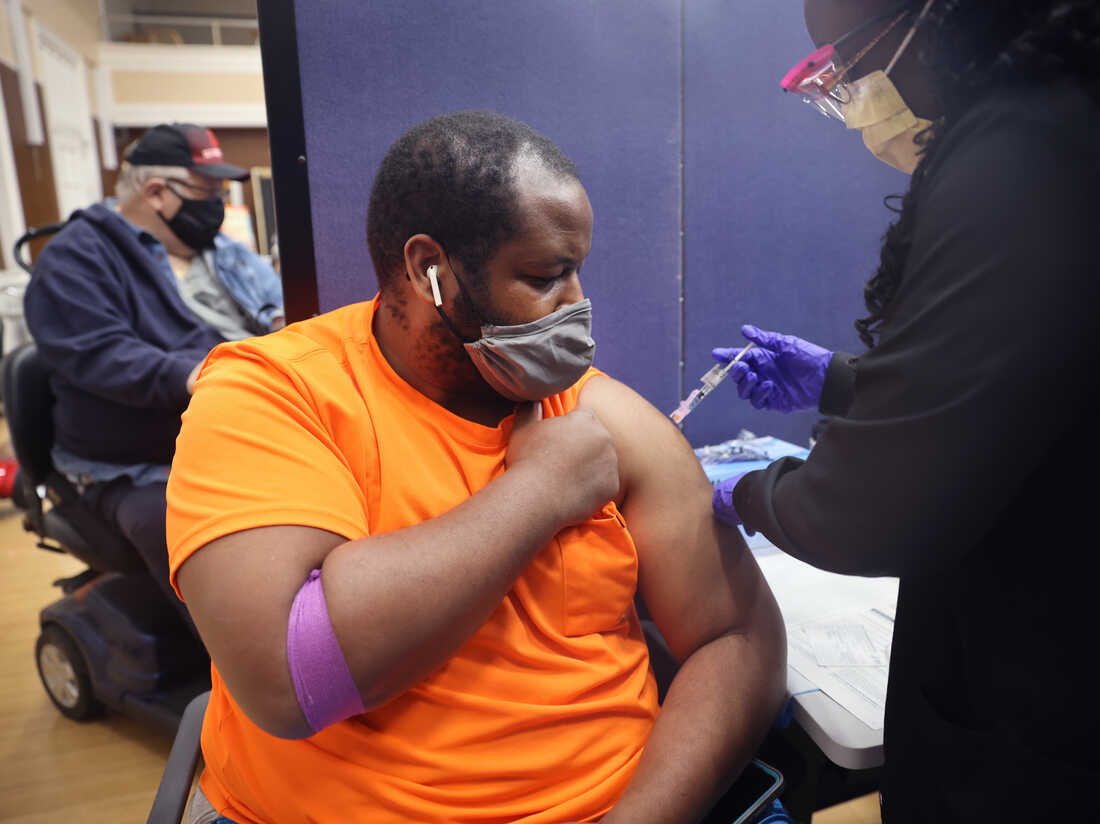
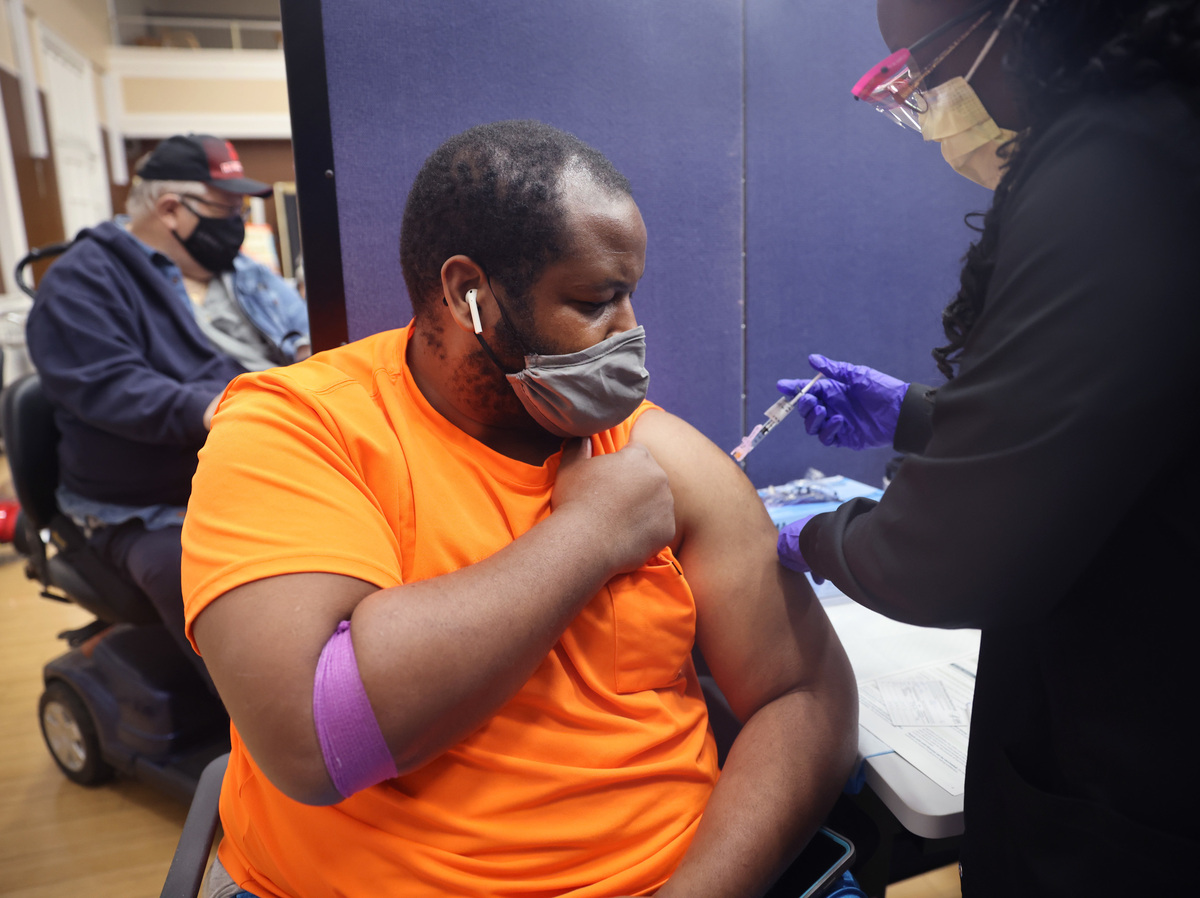
The No Surprises Act is intended to stop surprise medical bills. It could also slow the growth of health insurance premiums.
J. Scott Applewhite/AP
hide caption
toggle caption
J. Scott Applewhite/AP

The No Surprises Act is intended to stop surprise medical bills. It could also slow the growth of health insurance premiums.
J. Scott Applewhite/AP
Patients are months away from not having to worry about most surprise medical bills — those extra costs that can amount to hundreds or thousands of dollars when people are unknowingly treated by an out-of-network doctor or hospital.
The No Surprises Act — which takes effect Jan. 1 — generally forbids insurers from dropping such bills on patients and, instead, requires health care providers and insurers to work out a deal between themselves.
Some observers have speculated that the law will have the unintended consequence of shifting costs and leading to higher insurance premiums.
Many policy experts told KHN that, in fact, the opposite may happen: It may slightly slow premium growth.
The reason, said Katie Keith, a research faculty member at the Center on Health Insurance Reforms at Georgetown University, is that a new rule released Sept. 30 by the Biden administration appears to “put a thumb on the scale” to discourage settlements at amounts higher than most insurers generally pay for in-network care.
That rule, which provides more details on the way such out of network disputes will be settled under the No Surprises Act, drew immediate opposition from hospital and physician groups. The American Medical Association called it “an undeserved gift to the insurance industry,” while the American College of Radiology said it “does not reflect real-world payment rates” and warned that relying on it so heavily “will cause large imaging cuts and reduce patient access to care.”
Such tough talk echoes comments made while Congress was hammering out the law.
Here’s how the law will work and how it might affect insurance premiums and the health care industry.
Sending unsettled bills to arbitration
The No Surprises Act takes aim at a common practice: large, unexpected “balance bills” being sent to insured patients for services such as emergency treatment at out-of-network hospitals or via air ambulance companies. Some patients get bills even after using in-network facilities because they receive care from a doctor there who has not signed on with an insurer’s network.
Patients were caught in the middle and liable for