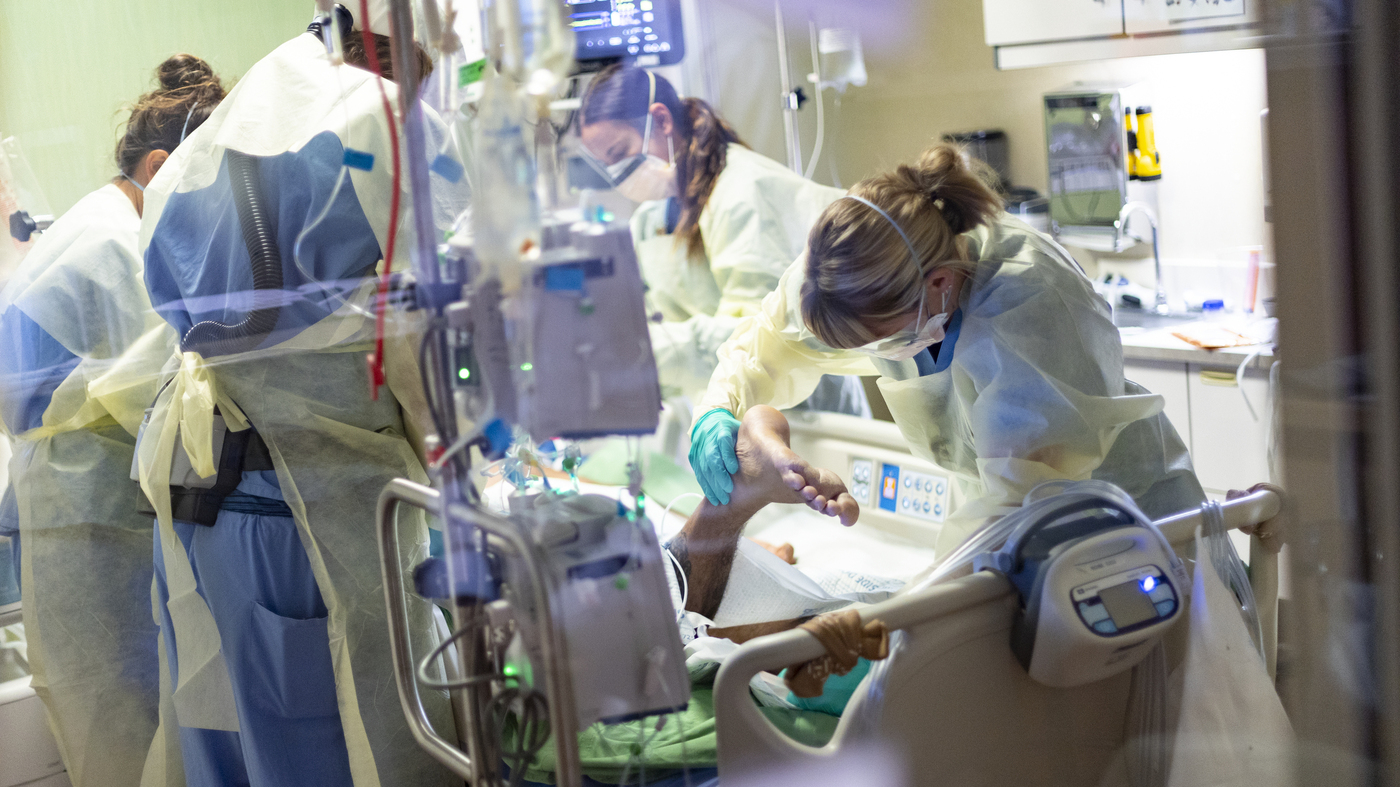
Expanded funds for in-home care can help seniors and disabled Americans stay in their homes. Here, Lidia Vilorio, a home health aide, gives her patient Martina Negron her medicine and crackers for her tea in May in Haverstraw, N.Y.
Michael M. Santiago/Getty Images
hide caption
toggle caption
Michael M. Santiago/Getty Images

Expanded funds for in-home care can help seniors and disabled Americans stay in their homes. Here, Lidia Vilorio, a home health aide, gives her patient Martina Negron her medicine and crackers for her tea in May in Haverstraw, N.Y.
Michael M. Santiago/Getty Images
For older people and people with disabilities, solving everyday practical problems can be the difference between being able to live at home or being forced to move to an institution. Sometimes people need help getting dressed or making meals. Sometimes they need help managing medications or shopping for groceries.
Originally, these things weren’t paid for by Medicaid, the federal health care program that many low-income and disabled Americans rely on. In recent years, the program has worked to expand coverage of home-based care but it’s still optional for states. Some states have adopted it widely, while in others, more care still happens in nursing homes and other institutions.
In April, the Biden administration rolled out funding from the American Rescue Plan to help states boost these services. And Thursday, the federal Department of Health and Human Services unveiled every state’s plan for how they’ll use the funds. An estimated $12.7 billion dollars in federal matching funds are available to “encourage states to expand home and community-based services and strengthen their programs,” according to an agency press release.

“More and more people are saying, if I need care, I’d like it to be done at home or here in my community versus an institution or a hospital or a nursing home,” says Health Secretary Xavier Becerra. “In the 21st century, we’re moving closer to a care model that’s based on giving people services in their home.”
Becerra adds that his own father spent his last few months in hospice at home. “When he passed, he was in my home, he was surrounded by family,” he says.
Medicaid recently surpassed 80 million beneficiaries — the most ever since the program was created in the 1960s. It is the primary provider of long-term care services for older people, since these are not covered by Medicare or private insurance.