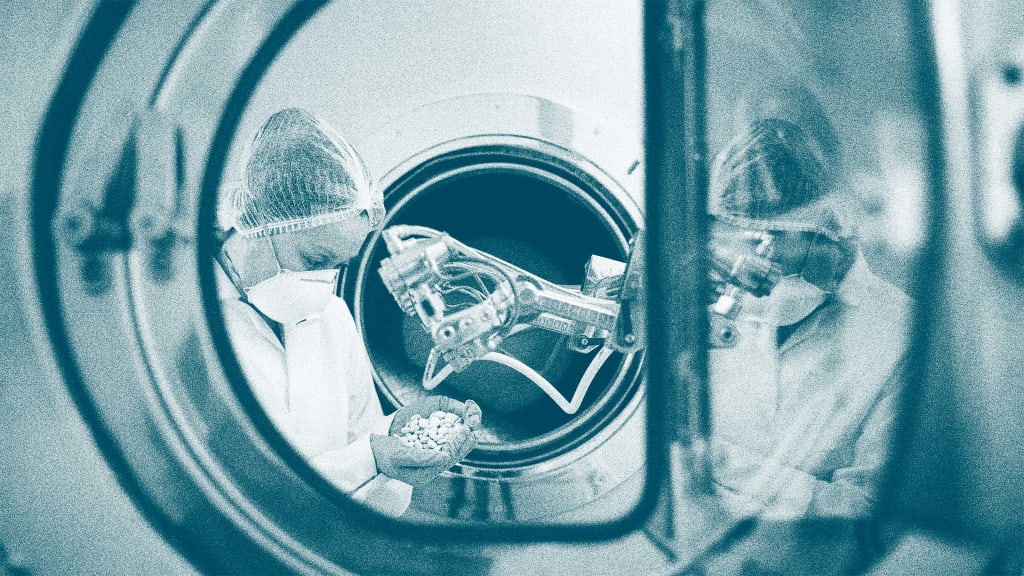
“The fourth industrial age is here,” says Daniel Kraft, a health care futurist and medical doctor. “It’s transforming how we get our digital banking done, how we stream movies. But health care is still stuck in the third — or maybe the second — industrial age, with fax machines and CD-ROMs.”
Specifically, innovations such as artificial intelligence and machine learning have been stubbornly slow to enter the health sector. And the big strides that have been made in data collection — wearables that monitor your vitals, voice biomarker trackers, and genomic sequencing, to name just a few — have so far resulted in only a few widely used, truly useful applications.
“Nobody wants more data, they want the actual insights that are useable,” says Kraft, who prefers the term now-ist to futurist. “How do we make actionable information that translates to the point of care or the bedside?”
Bob Wachter, chair of the UC San Francisco Department of Medicine and author of The Digital Doctor, remains optimistic that some of these new technologies may still have a significant impact. “Whether you’re looking at an X-ray, or trying to predict how many people are going to come to the emergency room next Tuesday, or seeing a patient and being reminded of an alternative diagnosis, A.I. will be useful in all sorts of ways,” he says. “I think it’s going to all work out. But it’s going to take far longer and be far bumpier than anybody anticipates.”
Here are five of the companies industry observers say are leading the charge down that bumpy road and reimagining the future of health care.
1. Youper
Youper designed its A.I.-based chatbot to guide users through the process of cognitive-behavioral therapy, supplemented with remote psychiatrists, health coaches, and an online pharmacy. The chatbot looks and feels like a standard text message exchange: patients talk about their thoughts and feelings and the A.I. responds with questions and advice, as programmed by mental health professionals.
“Some people say the chatbot is even better than talking to a human, because you can say how you’re truly feeling,” says Youper CEO Jose Hamilton. “[You might say,] ‘I’m feeling 100 percent angry’ or ‘100 percent depressed.’ And then the chatbot will start guiding you toward what’s making you feel that way.”
Youper does not intend to replace psychiatrists, but instead to allow them to see more patients than