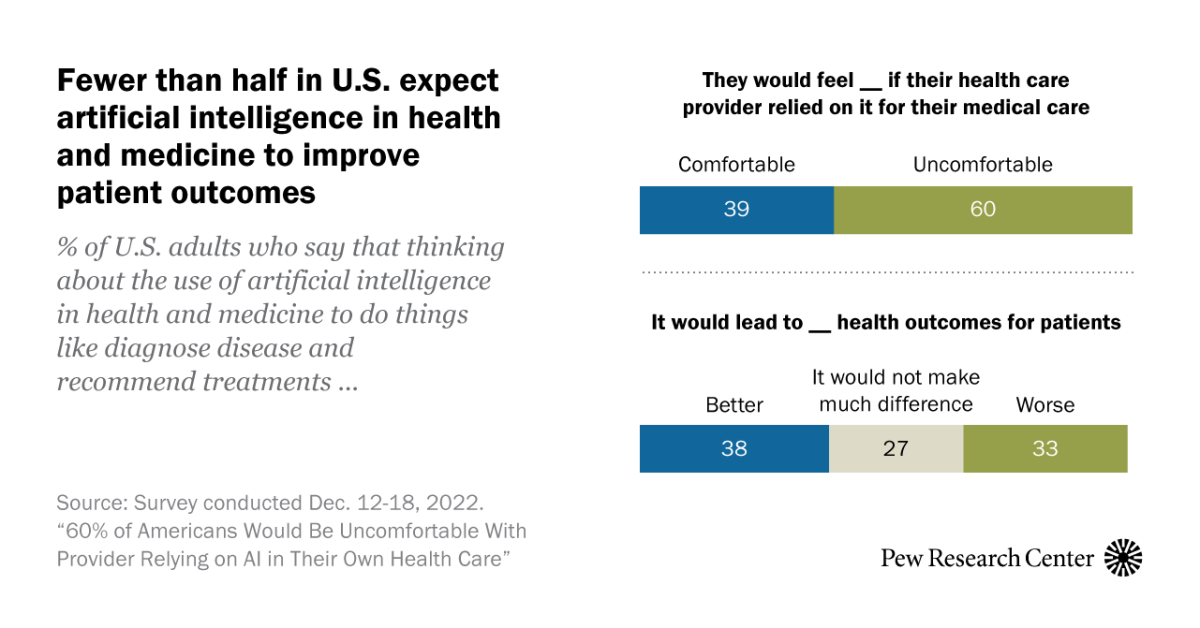
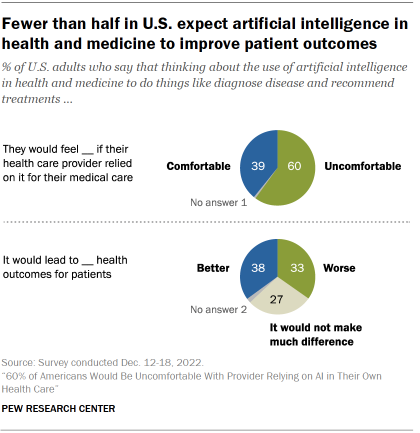
In medication, the cautionary tales about the unintended effects of artificial intelligence are by now legendary.
There was the application meant to predict when individuals would establish sepsis, a lethal bloodstream infection, that activated a litany of wrong alarms. An additional, meant to boost stick to-up treatment for the sickest sufferers, appeared to deepen troubling wellness disparities.
Wary of this sort of flaws, physicians have saved A.I. doing the job on the sidelines: aiding as a scribe, as a informal second viewpoint and as a back-place of work organizer. But the field has gained financial investment and momentum for utilizes in medicine and beyond.
Inside the Food and Drug Administration, which performs a essential position in approving new health care solutions, A.I. is a very hot topic. It is supporting to find out new drugs. It could pinpoint unforeseen aspect effects. And it is even getting mentioned as an aid to team who are overwhelmed with repetitive, rote responsibilities.
However in one very important way, the F.D.A.’s purpose has been subject to sharp criticism: how thoroughly it vets and describes the plans it approves to assist doctors detect everything from tumors to blood clots to collapsed lungs.
“We’re likely to have a ton of possibilities. It is remarkable,” Dr. Jesse Ehrenfeld, president of the American Medical Association, a foremost doctors’ lobbying group, said in an job interview. “But if physicians are likely to include these issues into their workflow, if they’re going to pay for them and if they’re likely to use them — we’re likely to have to have some self confidence that these resources function.”
President Biden issued an executive purchase on Monday that calls for polices throughout a broad spectrum of organizations to try out to manage the protection and privacy risks of A.I., together with in health and fitness treatment. The buy seeks much more funding for A.I. exploration in medication and also for a security software to acquire reports on hurt or unsafe procedures. There is a assembly with world leaders afterwards this 7 days to focus on the topic.
In an celebration Monday, Mr. Biden stated it was essential to oversee A.I. development and safety and make programs that people today can trust.
“For instance, to shield people, we will use A.I. to build cancer medicine that get the job done far better and charge much less,” Mr. Biden stated. “We will also