[UPDATED at 11 a.m. ET for news developments.]
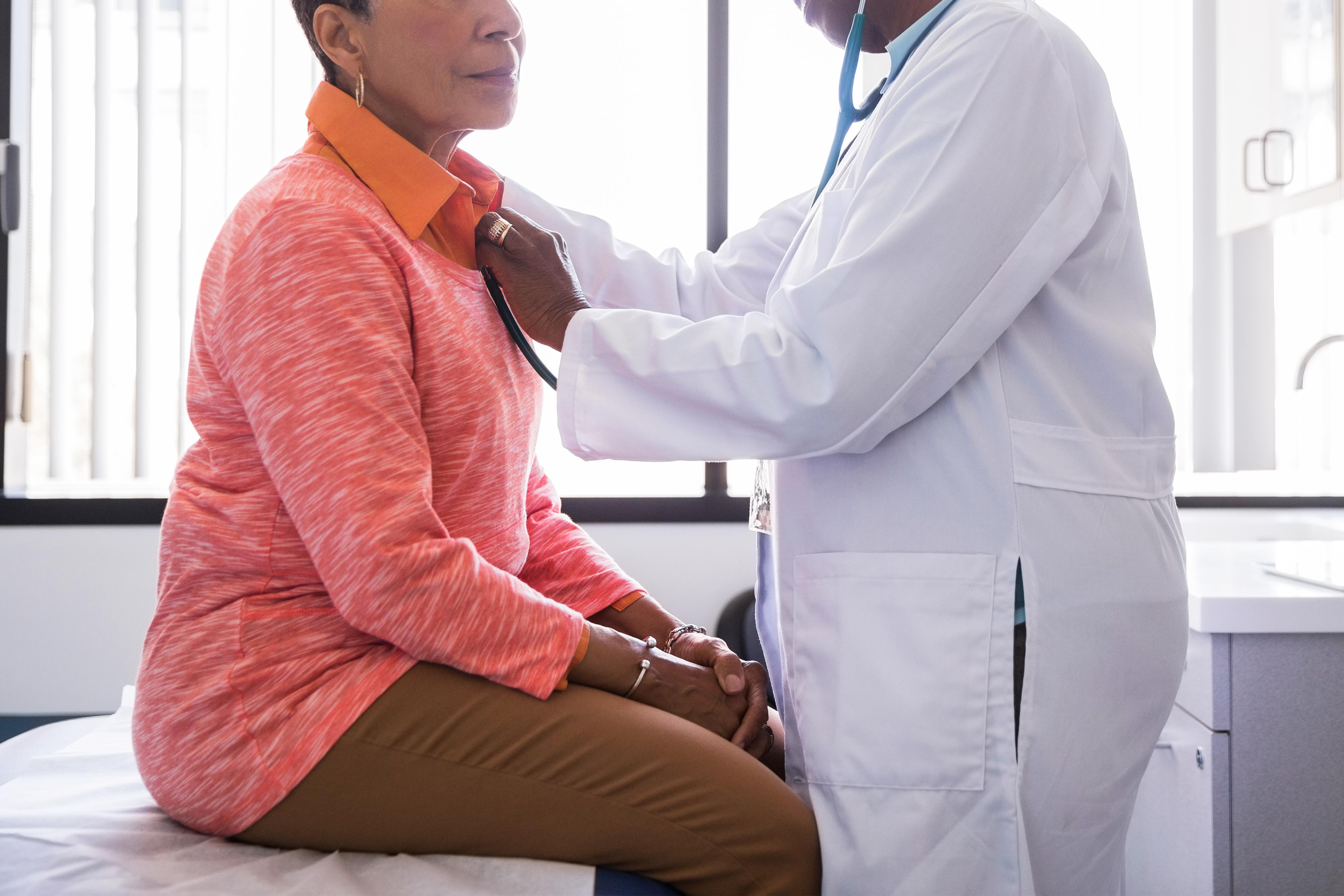
Doctors are urging Congress to call off cuts scheduled to take effect on Jan. 1 in the reimbursements they receive from Medicare.
In what has become an almost yearly ritual, physician groups are arguing that patients will have greater difficulty finding doctors who accept Medicare if lawmakers allow the pay cuts to happen.
A more than 4,000-page draft government spending bill released by lawmakers early Tuesday morning proposed much smaller-than-planned cuts to Medicare payments. But the bill, which Congress hoped to pass by the weekend to keep the government funded and avert a shutdown, would not go as far as doctors wanted.
“Despite overwhelming bipartisan, bicameral support to stop the full Medicare physician payment cut, Congress failed once again to end the cycle of harmful Medicare cuts, showing a disregard for vulnerable seniors,” the Surgical Care Coalition, an organization representing surgeons and anesthesiologists, said in a statement.
The doctors’ lobbying campaign had gained traction on Capitol Hill. A bipartisan group of 115 House lawmakers rallied behind doctors in a letter to congressional leaders and President Joe Biden last week, urging them to prevent cuts that they argued would “only make a bad situation far worse” for Medicare patients.
In recent years, the Centers for Medicare & Medicaid Services scheduled the pay cuts to offset the cost of increasing payments for underpaid services, like primary care. Physicians also stand to see reductions tied to broad cuts implemented by Congress in recent decades to try to control government spending.
Some Republicans have pushed to wait on passing the spending package until their party controls the House of Representatives next year and can have a greater say over what they call out-of-control spending. One priority of the incoming House Republican majority is curbing Social Security and Medicare, a federal health insurance program for people age 65 and older, among others.
“We’re mortgaging our kids’ futures,” Sen. Ron Johnson of Wisconsin, a Republican on the Senate Budget Committee, told reporters, referring to overall spending. “This is killing us from a financial standpoint. It’s got to stop.”
Despite concerns about ballooning government spending, for years doctors have been successful in delaying or softening proposed pay cuts, arguing that there would be dire consequences if the cuts kicked in.
Physicians carry a lot of political weight in Washington. The American Medical Association, the professional organization that represents and